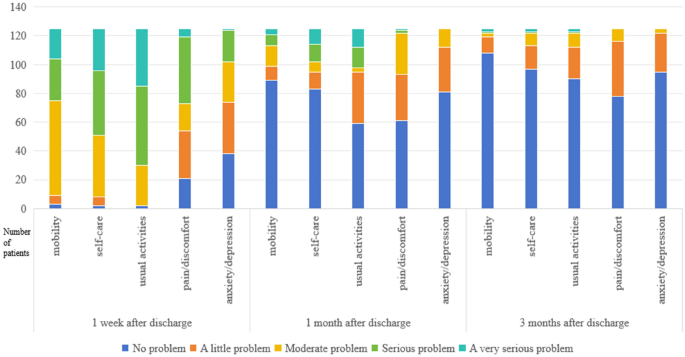
In the current research, a follow-up investigation into the QoL among 125 liver patients was conducted using the EQ-5D-5L questionnaire, and the potential determinants were meticulously examined. The findings revealed that the majority of patients had yet to regain mobility, self-care, and usual activities just one week post-discharge, and they continued to endure discomfort. It typically takes them around three months to reclaim their capabilities. On average, the duration of post-discharge pain was approximately four days. Other studies have indicated that the QoL of liver donors has notably diminished following surgery, and prolonged observation is crucial for enhancing patients’ QoL16. Moreover, the review of the literature revealed that patients who underwent fourth-level liver surgery demonstrated a superior QoL at 13 to 24 months and beyond three years post-operation compared to those who had less than a year’s worth of follow-up. However, the recovery process within the first three months post-surgery significantly impacts the long-term QoL of these patients17. Consequently, this study delved into a post-surgery QoL follow-up analysis for fourth-level liver surgery patients at the three-month mark. The data suggest that it’s imperative to bolster the patient’s rehabilitation efforts, focusing on mobility and daily activities during the critical first month following surgery, and to ensure they receive the necessary support to regain their independence promptly.
This research reveals that factors like gender, age, ethnicity, educational background, occupation, and BMI do not impact a patient’s QoL following their release from the hospital. Yuan Liao’s research delved into the QoL and its determinants for patients post-liver transplant, concluding that age, gender, and education level didn’t correlate with their QoL7. Similarly, Meimei Liu noted that there was no substantial statistical discrepancy in the EQ-5D UI among various subgroups, including gender, age, nationality, occupation, and education level18. The study’s findings indicate that the method of admission can influence a patient’s QoL for up to three months post-discharge, with emergency patients experiencing a lower QoL compared to those admitted through regular channels. Marital status, particularly for those who are divorced or widowed, can boost QoL within a week of discharge. The presence or absence of post-discharge pain affects QoL for a month, with pain-free patients enjoying a notably higher QoL. Previous studies have been sparse on the connection between admission methods and QoL. This study highlights a lower QoL among emergency department patients, which could be attributed to their critical condition and the array of diseases they often face, thus impacting their post-operative QoL. Studies have also shown that emergency surgeries, due to their urgency, are often rushed and have a higher risk of complications and mortality, leading to reduced quality of life post-surgery19. Moreover, pre-existing conditions such as hypertension, diabetes, lung disease, or heart disease can significantly increase the risk of post-operative complications20. We recommend that healthcare professionals give closer attention to emergency department patients and implement targeted interventions, such as pain management and early rehabilitation exercises. Furthermore, research indicates that marital status does not significantly influence the quality of life for patients undergoing fourth-level liver surgery.
Persistent pain is a major deterrent to the QoL for patients post-discharge, and it can severely hamper their recovery process. If acute pain during the initial phase of the perioperative period is not adequately managed, it may escalate into chronic post-op pain, significantly impacting the disease’s progression and outlook. Pain is a crucial factor contributing to the escalation of postoperative complications and mortality rates. Studies indicate that a 10% increase in severe post-op pain can lead to a 24% increase in pain intensity six months post-surgery21. Previous research has yet to fully delve into the correlation between pain and patients’ QoL. This study, however, offers fresh insights. It suggests that healthcare professionals must prioritize addressing the onset of pain in patients who undergo liver surgery and implement essential measures to mitigate their discomfort to prevent the onset of persistent pain upon discharge. For effective pain management in liver surgery patients, we recommend employing preoperative preemptive analgesia, such as the use of nonsteroidal anti-inflammatory drugs, in combination with postoperative multimodal analgesia, which involves a sequential approach to analgesics, complemented by non-pharmacological methods22.
link