There were 171 patients screened and five (2.9%) were ineligible (lacked capacity, n = 2; unable to speak English, n = 2; on concurrent antibiotics, n = 1). Of the remaining 166 patients, 61 declined to participate (unable to return for face-to-face review, n = 37; too many questionnaires, n = 5, unwilling to participate, n = 19). In total 105 (62.5%) participants were enrolled into the study, baseline characteristics are shown in Table 1. There were two procedures cancelled and no longer required, three perioperative deaths (two cardiac events and one pulmonary embolus) and one participant lost to follow-up, leaving 99 participants for analysis. SSI was diagnosed during face-to-face review in 22 participants (SSI rate 22.2%). Remote assessment correctly identified SSI in 20 participants (sensitivity; 90.9%), and those without SSI in 70 participants (specificity; 90.9%). The positive and negative predictive values for remote assessment were 74.1% and 97.2% respectively. The distribution of SSI severity was 14 (63.6%) mild, 4 moderate (18.2%) and 4 (18.2%) severe. Summary carbon emissions for face-to-face and remote assessment models are shown in Table 2.
Model one (standard of care): face-to-face review
The environmental cost (eC) related to face-to-face assessment across all participants totalled 4293.7 kgCO2e (range 31.1-75.8). Mean emissions per patient were 43.4±10.9 kgCO2e, 95% CI; 41.22-45.53. The return distance to clinic was 33.5±28.0 miles, and total distance travelled by all patients for face-to-face review 3312.2 miles (range 1.6-134.2 miles). Mean time to review patients was 13.7±5.4 minutes. The breakdown of emissions per resource type is presented in supplementary table 4.
Model two: remote first screening (RFS)
Assuming each patient with SSI required face-to-face review after their initial remote review, a RFS approach resulted in a total eC of 1,245.5 kgCO2e (range 1.2-77.2). Compared to a face-to-face model, RFS would result in a mean reduction of 30.8±19.2 kgCO2e per patient, 95% CI; 27.01-34.57 (face-to-face vs RFS; 43.4 vs 12.6 kgCO2e, relative reduction 71.0%, p < 0.001). For patients reviewed in a RFS clinic, carbon offsetting would be equivalent to CO2 sequestered by 1.24 trees/year. The return distance to clinic using a remote first screening model was 7.6±18.6 miles per patient, and the total distance travelled by all patients for face-to-face review reduced by 2461.2 miles (range 4.6-102 miles, face-to-face vs RFS 3312.2 vs 751.0 miles, relative reduction 77.3%). Using a RFS approach reduces mean review time by 6.8±7.0 minutes (face-to-face vs remote 12.5 vs 6.8 minutes, relative reduction 44.5%, p < 0.001).
Model three: remote first treatment (RFT)
Assuming each patient diagnosed with a mild SSI (requiring oral antibiotics) in a remote first treatment approach was managed in community, and those with moderate (requiring intravenous antibiotics) and severe (requiring surgical intervention and antibiotics) required face-to-face review, there would be a mean reduction of 38.5±15.8 kgCO2e per patient, 95% CI; 35.38-41.62 (face-to-face vs RFT 43.4 vs 4.9 kgCO2e, relative reduction 88.8%, p < 0.001). Each patient managed in this model would have a carbon offsetting value of 1.42 trees/year. The return distance to clinic using a RFT model would be 1.8±7.2 miles per patient, and total distance travelled by all patients reduced by 3135.6 miles (range 8.0-53.8 miles, face-to-face vs RFT 3312.2 vs 176.6 miles, relative reduction 94.7%). RFT reduces mean review time by 7.1±2.6 minutes (face-to-face vs remote 12.5 vs 5.5 minutes, relative reduction 56.0%, p < 0.001).
Cost analysis
Model one (standard of care) resulted in a total financial cost (fC) of £9,541.75 for the whole patient group, and mean fC of £105.31±41.5 (95% CI; 97.14-113.47) per patient. Using a RFS approach results in a mean fC per review of £45.13±69.03 (95% CI 31.53-58.73), a reduction of £60.17±42.98 (95% CI; 51.71-68.64, relative reduction 57.1%, p < 0.001) per patient. Total fC would be £4,468.22 (relative reduction compared to face-to-face £5,073.53, 53.2%). Mean fC per review using RFT is £22.02±40.58 (95% CI 14.03-30.02), a reduction of £83.29±45.51 (95% CI; 74.32-92.25, relative reduction 87.0%, p < 0.001) per patient. The total fC of applying RFT would be £2,180.22 (relative reduction compared to face-to-face £7,361.53, 77.2%).
Sensitivity analysis
As a sensitivity analysis, the mean (13.7 min) and median clinic review time (12.3 min) were varied within their respective 95% confidence intervals and applied to each model. The cost estimates ranged from £27.13-49.94 for RFS, and £12.92-26.02 for RFT (supplementary table 5). Mean (33.46 miles) and median (26.40 miles) patient travel distances were varied within their 95% confidence intervals and applied to each model for both cost and emissions estimates (Table 3).
Cost-Emissions Analysis
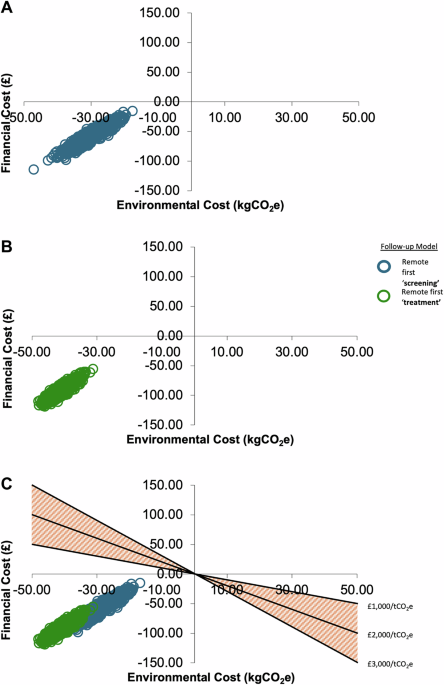
All remote first methods demonstrate reduction in both eC and fC compared with face-to-face standard of care irrespective of chosen model. Cost-emissions planes for each remote model are distributed to the bottom left axis indicating environmental and financial domination over a face-to-face model (Fig. 1A–C). As there is no accepted ceiling ratio threshold, a range are presented in Fig. 1C, indicating acceptance of all remote methods. Mean incremental cost-emissions ratios are not calculated due to the cost-emissions domination.
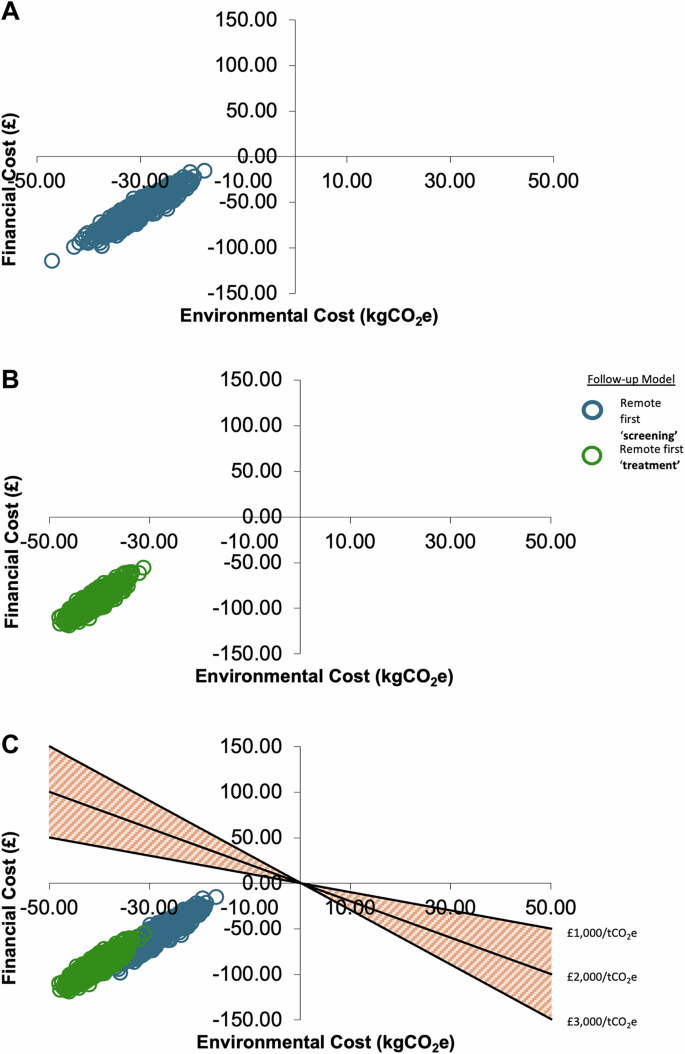
A–C Cost-emissions planes for remote follow-up models. A Remote First Screening. B Remote First Treatment. C All Remote Follow-up Models with possible ceiling thresholds for accepting environmental interventions are displayed.
Model Extrapolation
Scenarios were modelled to evaluate the impact of a change in practice varying postoperative review from 100% face-to-face to 100% remote assessment. There is a net benefit eC if 30% or more patients are offered RFS. This falls to just 10% of patients with RFT (Table 4). In 2022 there were 14,700 open vascular procedures in the NHS, United Kingdom (UK)11. No data are available to base the actual current proportions of in person or remote postoperative appointments, however general practice clinic-remote follow-up ratio is 7:312. Under this assumption, further implementation of remote models of postoperative care would produce estimated cost savings ranging £389,059,56-£728,792.89 and a reduction in carbon emissions of 267.4-380.7 tCO2e (938.2-1,335.8 trees. Looking across the entire NHS, 3,102,674 surgical procedures were performed in 202013. Extrapolating using the same clinic-remote follow-up assumption of 7:3 could enable cost savings ranging £82,117,344.50-£153,823,588.00 and a reduction in carbon emissions of 56,435.7-80,347.3 tCO2e (198,020.0-281,920.4 trees, Table 5).
link